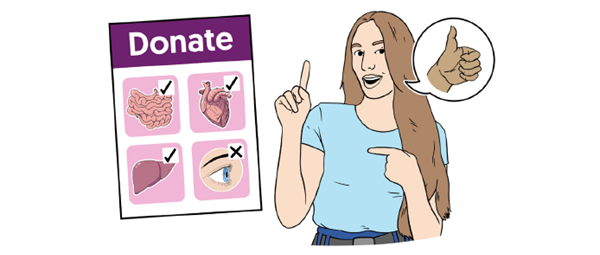
What is organ donation?

Read about organ donation on our website and think about what's right for you.
Register your decision on the NHS Organ Donor Register.
This will give your loved ones the certainty they need to support your choice.

Talk to your loved ones about what you've decided.
They will be expected to support your decision if you die in a way that means organ donation is a possibility, and clinicians will never proceed if your family objects.
Did you know?
Not many people die in circumstances that make it possible for them to donate their organs.
This is why every potential donor is precious.
What happens in the future

If you die in a way that means organ donation is a possibility, a specialist nurse will access the NHS Organ Donor Register to see if you had registered a decision.

The specialist nurse will discuss your decision with your loved ones, or if you hadn't registered a decision, ask your loved ones if they know your feelings about organ donation.
If a deemed consent or opt out system applies where you live, it will be considered that you are willing to become a donor, unless you’ve opted out or are in one of the excluded groups.

If you had registered a decision to donate, or your family inform the specialist nurse that it's what you would have wanted, you could go on to save up to nine lives.
If you had registered a decision not to become an organ donor, this will be respected.